- Home
- Treatments
- Conditions Treated
- Accelerated Healing – EMTT
- Acupuncture
- Physiotherapy For Children
- Diagnostics
- Dietitian
- Hands On Treatment
- Home Visits
- Hydrotherapy
- Injections
- Men’s Health
- Neuro Physiotherapy
- Rehabilitation
- Respiratory Physiotherapy
- Shockwave Therapy – ESWT
- Sports Therapy
- Women’s Health
- Microsuction Earwax Removal
- Information
- Contact
- Help Centre
- Home
- Treatments
- Conditions Treated
- Accelerated Healing – EMTT
- Acupuncture
- Physiotherapy For Children
- Diagnostics
- Dietitian
- Hands On Treatment
- Home Visits
- Hydrotherapy
- Injections
- Men’s Health
- Neuro Physiotherapy
- Rehabilitation
- Respiratory Physiotherapy
- Shockwave Therapy – ESWT
- Sports Therapy
- Women’s Health
- Microsuction Earwax Removal
- Information
- Contact
- Help Centre
ADVICE, SUPPORT,& TREATMENT
menopause
Specialist treatments & advice
Advice and Treatment for Women with Menopause.
Our practitioners are highly skilled in the treatment of many conditions related to menopause.
These include joint pain, headaches, sleep and weight gain.
Below are several treatments, and advice, that we can offer women going through the menopause.

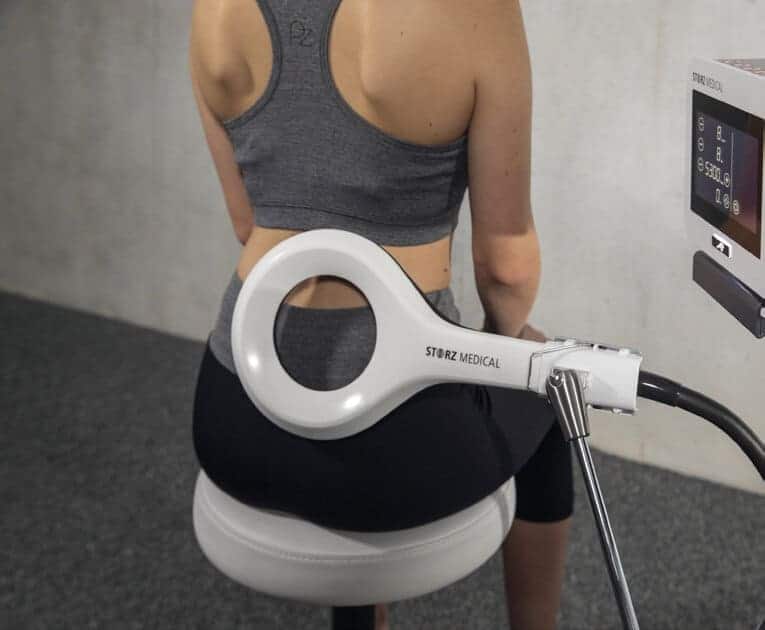
Solutions at The Physiotherapy Centre
How we can help
Conditions & solutions explained
Frozen shoulder is a condition mainly affecting women between the ages of 40 and 60 implying there are metabolic and hormonal influences involved (menopause).
The main symptoms of frozen shoulder are pain, progressive stiffness of the shoulder and reduced function. The time frame for frozen shoulder to improve is between 1 and 3 years.
There are 3 phases associated with frozen shoulder and treatment varies dependent on the phase you are in.
Phase 1 (freezing) is characterised by mainly pain and inflammation and injection therapy and EMTT (electromagnetic transduction therapy) are the treatments of choice. EMTT is innovative technology which helps the tissues to heal and repair by working at cellular level and improving local blood flow to accelerate tissue repair and reduce inflammation and pain.
Phase 2 (frozen) is characterised mainly by stiffness and a lack of function. In order to help with the stiffness manual therapy, focused shockwave therapy combined with rehabilitation is the treatment of choice. Focused shockwave therapy is a low intensity shockwave treatment to promote and accelerate tissue repair and healing. It has regenerative abilities therefore restoring the tissue back to it’s formal non painful state.
Phase 3 (thawing) is mainly characterised by ongoing stiffness and lack of function rather than pain and manual therapy combined with rehabilitation is recommended.
All these treatments are very safe and have been done to millions of people with no side effects apart from some transient discomfort.
Our treatment programmes can improve the journey of you suffering with frozen shoulder and help towards a full resolution of the problem. Often it is regarded as ‘self-limiting’ however research evidence suggest that only 39% of patients fully recover with 11% reporting ongoing functional limitation.
Our team is very experienced with this condition as it accounts for a large proportion of all shoulder pain as it affects 2-5% of the whole population with women more affected than men and is highly associated with diabetes (10-36%).
We can help to make the journey shorter and less painful, get full resolution of the problem and regain normal function of the shoulder.
Osteoporosis is a health condition that weakens bones, making them fragile and more likely to break. Losing bone is a normal part of ageing, but some people lose bone much faster than normal, which can lead to osteoporosis.
Women lose bone rapidly in the first few years after the menopause. They are more at risk of osteoporosis than men, particularly if the menopause begins early (before the age of 45) or they’ve had their ovaries removed (total hysterectomy).
Your genes are responsible for determining your height and the strength of your skeleton, but lifestyle factors such as diet and exercise influence how healthy your bones are.
Regular exercise is essential. Weight-bearing exercise and resistance exercise are particularly important for improving bone density and helping to prevent osteoporosis.
If you’ve been diagnosed with osteoporosis, it’s a good idea to talk to an expert before starting a new exercise programme to make sure it’s right for you.
Osteoporotic spinal fractures can be excruciatingly painful, but physiotherapy can help with pain relief. Both acupuncture and EMTT treatment can be effective tools for reducing pain, and once the pain subsides, restoring flexibility and strength is vital.
We can guide you through safe exercises, help with pain relief and educate you on how to manage your condition here at The Physiotherapy Centre.
Arthralgia or generalised joint pain is experienced by more then 50% of women around the time of menopause.
It can be difficult to determine the exact cause as it often coincides with the development of osteoarthritis and is thought to be as a result from a reduction in oestrogen levels. Oestrogen is the primary female hormone responsible for protecting joints and reducing inflammation, when oestrogen drops during the menopause inflammation increases and leads to painful joints.
At present there is no specific treatment for menopausal joint pain and hormone replacement therapy can be considered for women having joint pain and demonstrating other typical menopausal symptoms.
Physical exercise and weight loss has been shown to have positive effects on the joint pain especially if there is underlying osteoarthritis. Exercise helps to reduce the stiffness in the joints and is safe to do. It promotes strength around the joints and bones providing protection from the more long-term effects of alteration in oestrogen levels such as osteoporosis which results in an increased risk of broken bones.
Acupuncture and hydrotherapy are other treatments that can help to reduce the joint pains and acupuncture can also help with the other factors associated with chronic pain and menopause such as fatigue, poor sleep, sexual dysfunction and depression.
Tendon problems are often referred to in terms of tendinitis, tendinosis and tendinopathy. In essence these terms refer to different stages of tendon disease and associated timings.
Tendon related problems are more common in women than in men and typically in women between 40 and 60 years old as a result of hormonal changes.
Typical areas that become problematic are the gluteal (buttock area), achilles tendon, plantar fascia (a sheet of tissue on the sole of your foot), shoulder (calcific tendinitis) and elbow (tennis/golfers elbow).
Unfortunately, many of these tendon problems will become chronic in nature and can go on for months or years.
We are a specialist centre to treat these chronic conditions. We have specialist equipment to scan the tendons to identify exactly what is wrong with them and have innovative technology such as radial and focused shockwave therapy and EMTT (Electro Magnetic Transduction Therapy) to effectively treat them. It is a safe and approved treatment with up to 85% success rate.
As these tendons have become weak as a result of pain and reduced load capacity the shockwave therapy can help to activate the healing and regenerative process and careful rehabilitation is what will make the tendon strong again so you can get back to doing the activities and sports you enjoy.
Let’s be honest, having a good night sleep can really affect how you feel and function the next day. I know that all too well with having a three year old who didn’t sleep through the night until she was nearly one. Although mine was child related, I spoke to my mum pretty much on a daily basis who was also struggling sleeping, with her lack of sleep being related to the menopause. I really felt for my mum as I know myself the importance of a good night sleep. The NHS reports that most adults need between 6 and 9 hours of sleep every night. However, sleep disturbances during the menopause appear to be a very common complaint and appears not only to affect my mother, but at least 40 % of women. Right through from the perimenopausal stages to the postmenopausal; particularly affecting women aged in their late 40’s – 50’s.
Common factors that may play a role in this complaint appear to be vasomotor symptoms (hot flushes, night sweats, changes in blood pressure or heart palpitations), hormonal changes, exacerbation of primary insomnia and mood disorders. It has been found that some woman experience mood swings or low mood around the time of their menopause. With this in mind; I’m not surprised their mood swings can fluctuate. I know, (in fact my partner would definitely agree) that mine does too particularly if I haven’t had a good night sleep!
What can we try to help these symptoms?
Studies have shown that exercise may have a positive impact on our sleeping habits. A third of women felt that exercise such as jogging/evening walks had a positive impact. Exercise appeared to help ease falling asleep, deepness of sleep and a sense of sleep of wellness. Aerobic training also appears to be investigated and suggested this may help improve sleep quality and reduce hot flushes among menopausal woman.
The right exercise also has psychological benefits helping increase positive feelings and mental energy.
We may not be able to clear your menopausal symptoms, but we can definitely empathise and look at different exercise options that will help.
Many factors contribute towards headaches in both men and women. Women, however, often experience a relationship between headaches and hormonal changes and are 3 times more likely to suffer from migraines than men.
Fluctuations in female sex hormones can trigger several headache types including (most commonly) migraine, tension-type headaches and cluster headaches. Some women entering the menopause will experience headache for the first time in their lives, however menopausal headaches are most common in those who have suffered from headaches previously, especially around their menstrual periods.
Oestrogen withdrawal and hormone fluctuations are common triggers to worsening headaches leading up to menopause. This decline is not always consistent, hence resulting in more unpredictable, frequent and severe headaches during this time, especially if headaches were already linked to menstrual cycle. Taking HRT in some cases can help to prevent or better control headaches in some women, but can make matters worse in others.
In addition, other symptoms relating to the hormonal changes around this time- hot flushes/night sweats for example, result in poor sleep patterns, which adds to stress levels and therefore increases the likelihood of developing a migraine.
The hormonal cycle can even continue for some years after the last menstrual period-although the hormone changes are not sufficient to result in menstruation, they can still provoke headaches. For some women, migraines can improve when their menstrual cycles stop, but tension headaches often get worse.
Proven treatments for migraines/other headache types are often also effective for treating hormone related headaches/migraines. The National institute for clinical Excellence (NICE) approves the use of acupuncture in the treatment of various headache types including migraine and tension-type headaches. Typically, a course of up to 10 sessions of acupuncture over 5–8 weeks is recommended.
Acupuncture is known to be as effective as conventional drug preventative therapy and to be safe, long-lasting and cost-effective in the treatment/prevention of migraine (6). It can help in the treatment of migraine by providing pain relief (by affecting the levels of endorphins, serotonin and other chemicals in the brain and spinal cord), reducing inflammation and causes changes in blood flow, both intra- and extracranially.
There is also evidence that acupuncture is effective for a variety of menopausal symptoms including migraine, hot flushes/night sweats and insomnia. As well as the effects mentioned in the previous paragraph, acupuncture is thought to have an effect on peri-menopausal/menopausal headaches as it increases oestrogen, especially estradiol, progesterone, prolactin, and other hormones.
Acupuncture is used regularly at The Physiotherapy Centre in the treatment of a variety of headache types, including those associated with hormonal changes. Patients reporting improvements in both the severity and frequency of their headaches, as well as resulting in them being able to rely less heavily on analgesic medication.
Benign Paroxysmal Positional Vertigo (or BPPV) is the most common cause of vertigo, which is a false sensation of spinning. It occurs when some of the calcium carbonate crystals (otoconia) that are normally embedded in gel in the inner ear become dislodged and migrate into one or more of the fluid-filled ear canals, where they are not supposed to be. It causes episodes of vertigo, triggered by movement and changes in position.
The incidence of BPPV increases with age and many investigations have found it to be more common in women. Clinical experience has shown that BPPV can develop due to increased hormonal fluctuations, especially during menopause.
The good news is that BPPV can be effectively treated with the appropriate mechanical manoeuvers performed by a qualified healthcare professional, and this is something we can offer at The Physiotherapy Centre.
A lot of the information above will result in enhanced wellness and an improvement in mental health when going through menopause. Our experienced practitioners have many effective ways to treatment the many symptoms associated with menopause.
These treatments and the benefits they bring can have a hugely positive effect on the wellbeing of women during menopause.
menopause
made better with
our solutions
our assurance to you
Experienced practitioners
Our practitioners have many years of experience.
Latest advice & Techniques
All our practitioners are trained to the latest and highest standards.
Safe
We operate in a safe and clean environment.
Discretion Assured
We will always ensure that your privacy and discretion are of the highest importance to us.
book online today
The quickest and simplest way to make your appointment is online.
Get In touch
Send a message to us, and we’ll get right back to you
We believe in all people achieving their full potential for health and well-being.
