Shoulder Osteoarthritis

Arthritis means inflammation of the joints. Osteoarthritis (OA) is the most common form of arthritis in the UK. OA mainly affects the joint cartilage and the bone tissue next to the cartilage.
Get A Fast Appointment
or Call
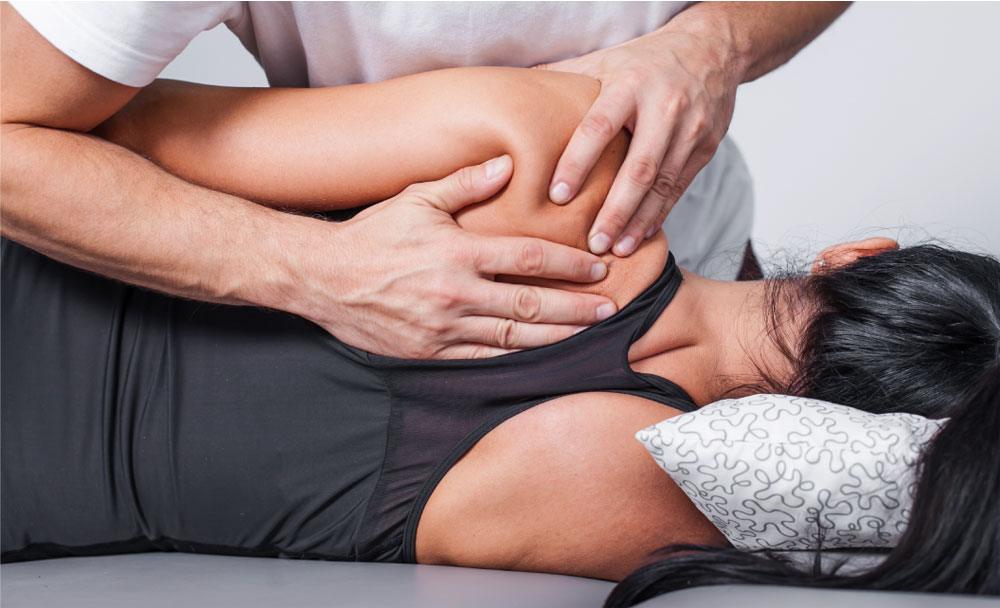
What causes osteoarthritis?
All normal joints and joint tissues are constantly undergoing some form of repair due to damage to the joint and surrounding tissues through stress and force that is placed on them in our daily activities. However, in some people, it seems that this repair process becomes faulty or delayed in some way and OA develops. In joints with OA, the joint cartilage becomes damaged and worn. The bone tissue next to the cartilage can also be affected and bony growths can develop around the joint edges. These growths are called osteophytes and may be seen on X-rays. The joints and the surrounding tissues can also become inflamed. This inflammation is called synovitis.

Factors that may play a role in the development of OA
Age: OA becomes more common with increasing age. By the age of 65, at least half of people will have some OA in some joint(s).
Genetics: There may be some inherited tendency for OA to develop in some people.
Obesity: Shoulder OA is more likely to develop, or be more severe, if you use your arms for weight-bearing e.g. pushing up from a chair or using walking aids.
Your gender: Women are more likely to develop OA than men.
Previous joint injury, damage or deformity: This may include previous joint infection, a previous fracture (break in the bone) around a joint, or a previous ligament injury that caused a joint to become unstable.
Occupation/Sport: Shoulder issues are more prevalent with people who use their arms above shoulder height in a repetitive or sustained way, especially when heavier loads are involved.
Posture: Becoming stooped and round shouldered puts more stress on the shoulder joint when performing normal movements.

Symptoms of osteoarthritis
-
In some cases no symptoms may occur. Quite a number of people can have X-ray changes that indicate some degree of OA but have no, or only very mild, symptoms.
-
Pain, stiffness, and limitation in full movement of the joint are typical. The stiffness tends to be worse first thing in the morning but tends to loosen up after half an hour or so.
-
Swelling and inflammation of an affected joint can sometimes occur.
-
An affected joint tends to look a little larger than normal. This is due to overgrowth of the bone next to damaged cartilage.
-
If you have bad OA that affects your shoulder, you may have difficulty in putting your clothes on, and using the arm above shoulder height
-
Pain at night may be an increasing problem with advancing OA


Do I need any tests?
Osteoarthritis can often be diagnosed based on your age, your typical symptoms and examination of your affected joints. Tests such as X-rays or blood tests are usually not needed.
What is the outlook for people with osteoarthritis?
The severity of symptoms can vary. In many people, OA is mild and does not make you any more disabled than expected for your age. However, in some people, the severity of OA and the disability it causes is out of proportion to your age.
What are the aims of physiotherapy?
The aim of physiotherapy is to increase joint mobility, improve muscle strength and try and relieve pain.
-
Pain relief:
Acupuncture and Dry Needling
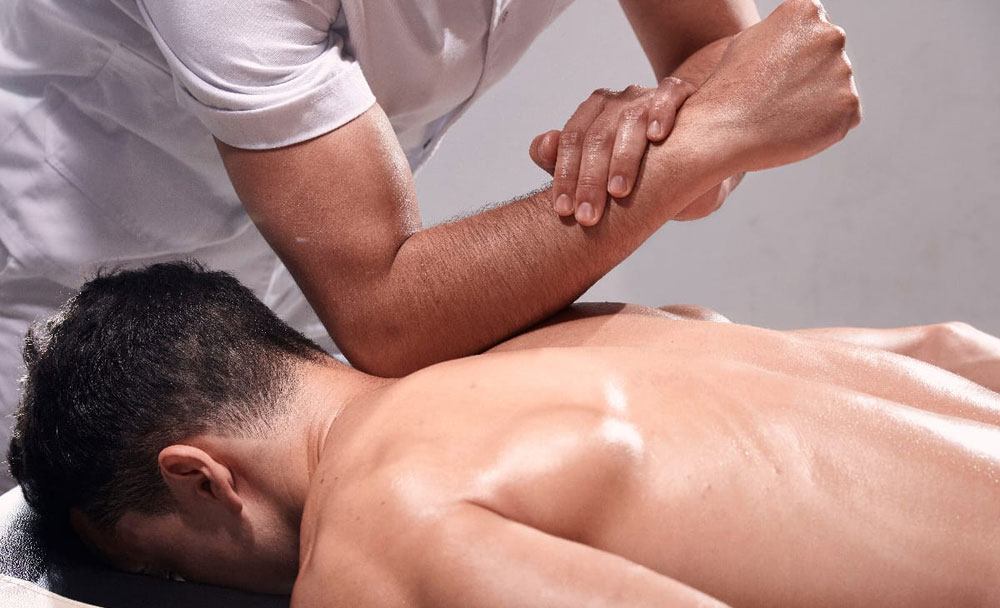
Soft Tissue Massage
Shockwave Therapy
EMTT
Injection Therapy -
Longer term rehab:
Education
Exercise prescription (home exercises, hydrotherapy, gym rehab)
In the most severe cases shoulder surgery is required. We offer a specialist service with regards to the long term rehabilitation following any surgery that is required.
Post-surgical physical therapy:
-
Ensuring your safety as you heal. You will perform specific activities and exercises at the correct time to allow for optimal healing. Restorative and reconstructive options may take several months to heal, with longer precautions.
-
Aiding motion of the shoulder. After surgery, your shoulder will be sore and swollen, and you may not feel like moving your arm. However, gentle motion is often recommended. Our experience and close working with many orthopaedic surgeons mean that we can choose the best options for recovery and guide you through the process.
-
Strengthening the shoulder. Due to prior disuse or postoperative pain, your muscles may not be as strong as normal. If the muscle was repaired during surgery, you will have to let it heal for a period of time, and we can let you know what activity is safe to help the healing along.
-
Relieving your pain. Using hands-on therapies and other modalities, we can help reduce your pain during exercise and daily activities.
-
Getting back to work and activities of daily living. Returning to work and daily activities may be slow, and your physio will guide you through the process to achieve the best results.
What Our Clients Say…
You Ask, We Answer
What is the cost of physiotherapy?
Find out about the costs of the initial assessment and follow up sessions of MSK physiotherapy.
How long is a session of physiotherapy?
A top question is about how long the sessions are, here we explain about the length of MSK initial and follow up sessions.
Do I need a referral to be treated by you?
To get your treatment at The Physiotherapy Centre, do you need to get a referral from your GP or Consultant?
